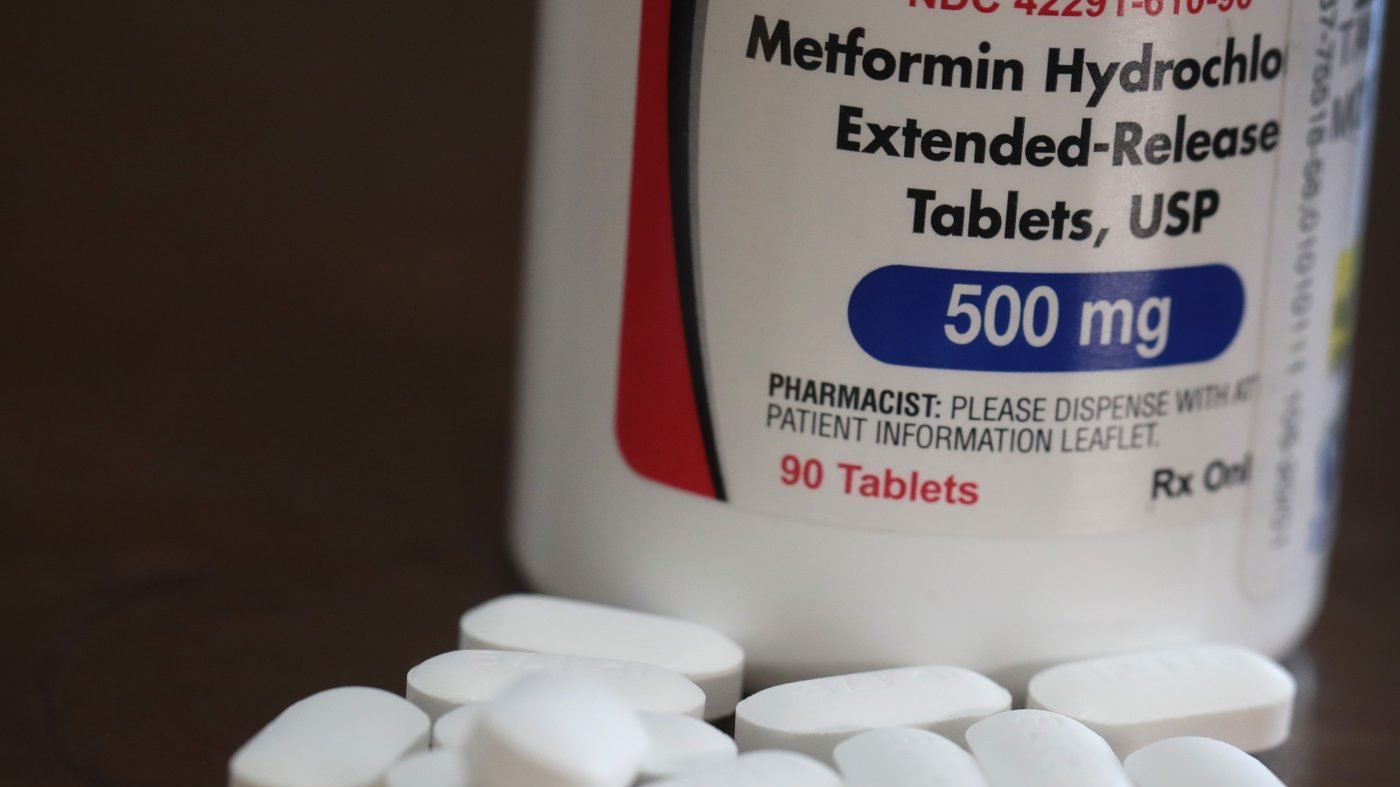
For over six decades, metformin has served as a foundational therapy for Type 2 diabetes, prescribed to millions worldwide. The prevailing scientific consensus held that its primary mechanism worked directly on the liver to reduce glucose production. New research published in Science Advances now fundamentally challenges that view, revealing a significant and previously unrecognized brain-based pathway central to the drug's efficacy.
A Brain-Centric Discovery
A research team led by Dr. Makoto Fukuda at Baylor College of Medicine has identified that metformin's ability to lower blood glucose depends critically on its action within a specific region of the brain known as the ventromedial hypothalamus (VMH). "We looked into the brain as it is widely recognized as a key regulator of whole-body glucose metabolism," said Fukuda, the study's corresponding author. The findings suggest that for decades, the drug has been engaging central nervous system circuits without clinical recognition.
The Role of Rap1 Protein
The study pinpointed a protein called Rap1 within the VMH as the crucial mediator. Researchers found metformin suppresses Rap1 activity, and this suppression is necessary for the drug's glucose-lowering effects at standard clinical doses. In genetically engineered mice lacking Rap1 in the VMH, low-dose metformin failed to improve blood sugar levels, even when the animals were on a high-fat diet designed to simulate Type 2 diabetes. Notably, other common diabetes treatments like insulin and GLP-1 agonists remained effective in these mice, confirming the specificity of the metformin-Rap1 pathway.
Further experiments demonstrated the brain's extraordinary sensitivity to the drug. When researchers delivered micro-doses of metformin directly into the brains of diabetic mice—amounts thousands of times lower than a standard oral dose—blood sugar levels dropped significantly. "We found that while the liver and intestines need high concentrations of the drug to respond, the brain reacts to much lower levels," Fukuda explained. This sensitivity points to a potent, targeted mechanism.
Implications for Treatment and Research
The discovery carries profound implications for the future of diabetes therapeutics. Most existing medications do not target the brain, meaning metformin has been operating through a unique channel. The identification of the Rap1 pathway in specific SF1 neurons within the VMH provides a clear biological target for developing new, more precise drugs. "These findings open the door to developing new diabetes treatments that directly target this pathway in the brain," Fukuda stated.
Beyond diabetes management, the research may shed light on other areas of study involving metformin. The drug has been investigated for potential benefits in conditions like brain aging and cognitive decline. Fukuda's team plans to explore whether the same Rap1 signaling mechanism underpins these broader effects. This line of inquiry reflects a growing scientific focus on the interconnectedness of metabolic and neurological health, a nexus with significant implications for public health policy and systemic healthcare responses to chronic disease.
The study, conducted in collaboration with institutions including Louisiana State University and Nagoya University in Japan, was funded by the National Institutes of Health, the American Heart Association, and the American Diabetes Association. It represents a significant shift in a field where research funding and scientific priorities are often subjects of intense political and budgetary debate.
This revelation about a cornerstone medication underscores how basic scientific research can upend long-established medical paradigms. As the global burden of diabetes continues to rise, understanding the precise mechanisms of effective treatments becomes ever more critical for developing next-generation therapies and managing one of the world's most pervasive chronic health challenges.