Health officials across the country are raising alarms as syphilis rates climb sharply, reversing years of progress against other sexually transmitted infections. New York alone has seen a fivefold increase in cases since 2013, according to local reports, and the trend is national.
Data from the Centers for Disease Control and Prevention shows congenital syphilis—transmitted from mother to baby during pregnancy—has surged 700% compared to roughly a decade ago. The disease can cause miscarriage, stillbirth, or infant death, and babies who survive may be born with deformed bones or organs.
While infections like chlamydia and gonorrhea have declined, congenital syphilis has risen for 12 consecutive years through 2024, the latest year of CDC data. The prevalence has reached its highest point since 1994.
The CDC has set a target of reducing syphilis rates among reproductive-aged women to 4.6 per 100,000 people by 2030. To meet that goal, the agency recommends that healthcare providers screen everyone aged 15 to 44 in areas with high disease rates. Testing should also be repeated during pregnancy in the most affected counties.
A new CDC map identifies U.S. counties where syphilis prevalence exceeds the 4.6 per 100,000 threshold. In those shaded areas, the agency advises testing for all sexually active individuals in that age range to curb further spread. Counties in white still have lower rates, but testing is recommended based on individual risk factors and symptoms.
“For many people, the most significant risk factor for syphilis is living in a community with high rates of syphilis,” the CDC noted.
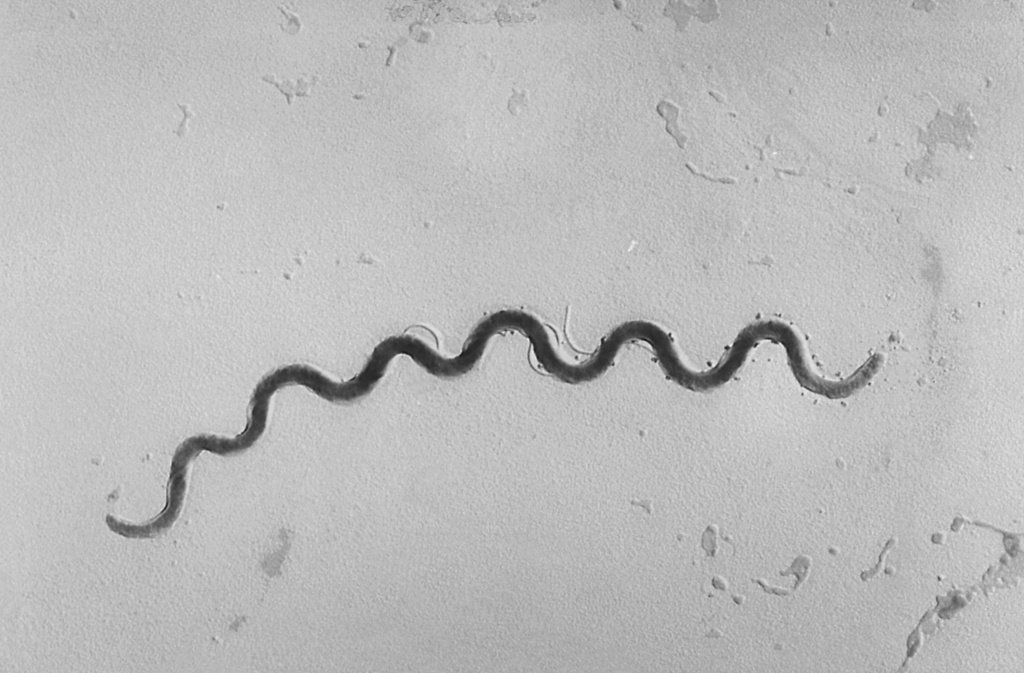
Dr. Lazarus Gehring, medical director of the Broome County Health Department in New York, described the infection as “kind of complicated,” pointing to its multiple stages and asymptomatic phases. The disease is caused by bacteria and typically presents with painless ulcers two to six weeks after exposure, said Dr. Khalil Ghanem, a Johns Hopkins Medicine professor. These ulcers may clear on their own, but without antibiotics, the infection progresses to secondary syphilis, where bacteria multiply and cause fever, skin lesions, and more.
The immune system can suppress symptoms again, leading to latent syphilis. “Sixty percent of people with latent syphilis will never have symptoms again. The other 40% suffer devastating complications including neurological problems, cardiovascular issues, and inflammatory masses all over the body,” Ghanem explained. “Overall, 10% of patients who are not treated for syphilis wind up dying from this infection. Syphilis is a cruel disease.”
Early treatment with penicillin or other antibiotics is critical and can cure the disease. The CDC’s push for widespread screening comes amid broader debates over public health funding and access to care. As policymakers weigh redirecting health dollars to patients ahead of 2026 reforms, the syphilis surge highlights gaps in preventive care, particularly for low-income and rural communities.
The data also underscores disparities that have long concerned public health experts. In a political climate where Black voters' decades of loyalty meet a debt Democrats refuse to pay, the disproportionate impact of STDs on minority populations remains a flashpoint. Meanwhile, as tech layoffs hit their highest level since 2023, the strain on state and local health budgets could worsen the crisis.
For now, the CDC’s map offers a clear warning: syphilis is back, and it's spreading. The question is whether the political will and resources will follow to contain it.